CC: vomiting
HPI: 83yo M w/ h/o IDDM, HTN, CHF, prior iatrogenic esophageal perforation w/ resultant fundoplication and neoesophagus 40yrs ago now presents to the ER c/o 3d of progressively worsening nausea, vomiting, and mild abdominal pain. Pt is A/Ox4, appropriate, in no active distress, but appears very thin. On coumadin
VS: 127/64, p67 (nsr), r14, sat99%ra, Tmax 36.9r
PE:
- Gen - comfortable, A/Ox4, cachectic
- HEENT - PERRLA, EOMI, no conjunctival pallor, non-icteric, no sublingual jaundice
- Neck - TM, supple
- CV/Resp - RR, NSR, no MRG/CTAB, no RRW, no adventitious lung sounds
- Abd - Mild LUQ TTP w/o rebound, no surgical Murphy's, no RT/G, non-peritonitic abd, guiac negative
- Neuro - No focal deficits
Assess: Elderly gentleman with likely bowel obstruction vs volvulus vs paralytic ileus, less likely infectious etiology, unlikely acute surgical abdomen
Plan: Labs, lactate, upright CXR and obstructive plain films (stat), CT A/P w/o contrast (stat)
Films unremarkable for acute pathology, no e/o free air, possible obstruction, no e/o volvulus.
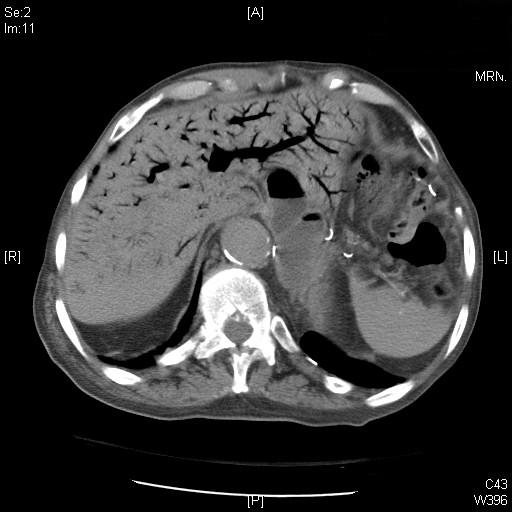
WOW!!! WTF?!?!
So what do you see? It's badness, plain and simple. Dr. Omi had mentioned that this is the most intrahepatic air she had EVER seen. Can you tell if it's biliary or venous?
It's venous, which Dr. Omi pointed out you can distinguish by the degree that the intrahepatic air extends to the periphery or the liver, whereas intrabiliary ductal air would be more concentrated to the middle. The next thing you should notice is the intraluminal free air throughout the bowel, indicating meseteric ischemia/infarction.
This gentleman was started on fluids, had a central line placed, BS Abx, and sent to the MICCU in stable condition. Lactate was 0.8, WBC 11, pH 7.34, bicarb 24. This was a gentleman that lulled us to sleep with his lack of pathology at first.
Bottom line: Elderly people with abdominal pain and vomiting are almost NEVER benign, no matter how benign they are.